Christmas is over. And a very different Christmas to boot. I am back in Norway, probably the most quiet and peaceful country in the world. Back to snow and ice and winter darkness. Back to a place where catastrophe and tragedy are strangers to most and familiar only to the few.
The contrast could not be greater to Bangladesh where I spent Christmas and New Year. Near the border to Myanmar, in the far east corner of Bangladesh, in one of the poorest parts of the country, a refugee camp has sprung up that is most likely the largest in the world. 850 000 people – men, women and children – live under conditions that can only be described as abominable. Some of them have lived there since 1994 when the first wave of refugees spilled across the border from Myanmar. The great majority has arrived since august when the violence in their home country forced them to pack up and flee. I had seen the footage of the exodus on TV before leaving and I had seen the photos of the refugee camp stretching for miles and miles across the once wooded hills of Chittagong province.

But actually taking it in with my own eyes, walking among the shelters in the mud and the dirt, taking in the smell and the stench, leave an impression that no camera or video can capture: This is no natural disaster, no earth quake or storm. This calamity is man-made. The realization is chilling and it makes my heart sink.
The Field Hospital
The Field Hospital where I work is set up across the road from the refugee camps and is run by Bangladesh Red Crescent, Norwegian Red Cross and Finnish Red Cross. Several other national societies provide staff, namely New Zealand RC, Hong Kong RC, Icelandic RC, German RC, Indonesian RC, Swedish RC and Swiss RC. It is located in a rubber tree plantation, hence the name: Rubber Garden Field Hospital. When I arrive it has been running for the better part of two months. The first rotations had to build and work under desperate conditions, battling the monsoon, the forbidding heat and the suffocating humidity. They had to cope with mud and flooding and disease and they had to push themselves to breaking point on several occasions; gravel had to be imported from India. An outbreak of measles and diphtheria, with the need for screening and isolating patients, threw the entire setup in disarray and put a new and unforeseen strain on hospital resources. More stringent visa policies lead to delays in delegate deployments and for several days there were only 3 GP’s doing all the work. No surgeon, no obstetrician, no anesthesiologist.

The main gate and the out-patient department at Rubber Garden Field Hospital
Standing on the shoulders of the teams before us, the working conditions of my rotation are comparatively charmed. Everything is set up and in place. I just need move in my tent, put up my mosquito dome and get to work. Within days almost all vacant positions are filled: I will do the surgery, we have an anesthesiologist, a gynecologist and three GPs. The climate has changed considerably, too, temperatures are below 30 degrees Celsius during the day and the nights are actually quite chilly. December is generally regarded to be the most pleasant month in Bangladesh. The humidity is bearable and the rains have largely ceased. This is a welcome breather for the staff at the field hospital and first and foremost for the people in the camps.

Patient transport is based on “strong people”, a term regularly used on the radio calls (Photo: Jane Heggie)
Work
But the flow of patients does not cease and we have our hands full all day and quite regularly until late in the evening. There are no Saturdays, Sundays or other holy days, no Xmas holidays or New Year’s day. The medical team – doctors, nurses and technicians – have to cope constantly with challenges that we are not used to from home. Measles and diphtheria are largely extinct in the Western world, but here the patients keep coming. I have to go back to my books from medical school to refresh my memory about these diseases and about the complications that can kill your patients, particularly children. Most of them are malnourished and when the epidemic broke out some died despite good supportive treatment. We are blessed to have a pediatrician, Siri, on the team and her contribution is invaluable. A huge vaccination campaign is being conducted in the camps, but vaccination coverage is still far from sufficient to prevent new infections. It is heartbreaking to see these children suffering, particularly when you know that something as simple and cheap as a measles shot could have prevented it all. We all have the same thought: It would be great to take the anti-vaccination campaigners back home on the evening ward round in the children’s ward! Maybe this sobering rendezvous with reality would change their minds.

Evening ward round in the children’s ward.: A definite cure for the anti-vacciners back home
I have been on two missions before, and both there and at home I’m used to getting a smile back when I smile to patients. This is rarely the case here. The kids, of course, do smile and laugh and giggle – kids are kids after all. But the adults – fathers, mothers and other relatives – usually don’t. This has bothered me a great deal. Is it a religious or cultural thing? Is it a consequence of the traumatic events they had to live through during these past months? Possibly, and for many quite likely so. But I have the suspicion that this reaction, or rather the absence of a reaction, is something altogether more sinister: These people, who have been oppressed and prosecuted and discriminated against for generations, probably find the idea completely alien that someone who is not from their family or tribe would show them normal kindness, treat them as equals, treat them with respect. Their collective memory has no recollection of such a concept. It just simply doesn’t cross their mind.

Kids are kids. In the outskirts of the refugee camp, in a swampy rice paddy, they play soccer!
There are countless difficult and complicated births and normal deliveries are the exception. The number of stillbirths outnumber live births, because – as is far too common in these parts of the world – people wait with consulting a doctor until their condition is far advanced, often beyond saving or cure. Many babies have been dead in the womb for many days when they finally come to us. Stefanie, our German gynecologist, and her excellent team of midwives have to make tough decisions every day, but cope brilliantly with whatever turns up on the door steps of maternity ward. Their stoic professionalism is inspiring. Having a gynecologist on the team is something I don’t ever want to be without on my next missions!
The surgical workload consists largely of burns, fractures and infections. And this again means rarely fresh burns, fractures or infections but large abscesses and burns that are typically seven to ten days old. The operating conditions are semi-sterile at best and every operation means potentially new infections. Patients are usually fasting when we see them in the out-patient department during the day because they only eat breakfast in the morning and this, very often, is their only meal for the day. The resulting malnourishment has of course serious consequences for their ability to heal and to fight infections. Bone fractures regularly take at least twice as long to mend as is common in the Western world or they don’t heal at all.
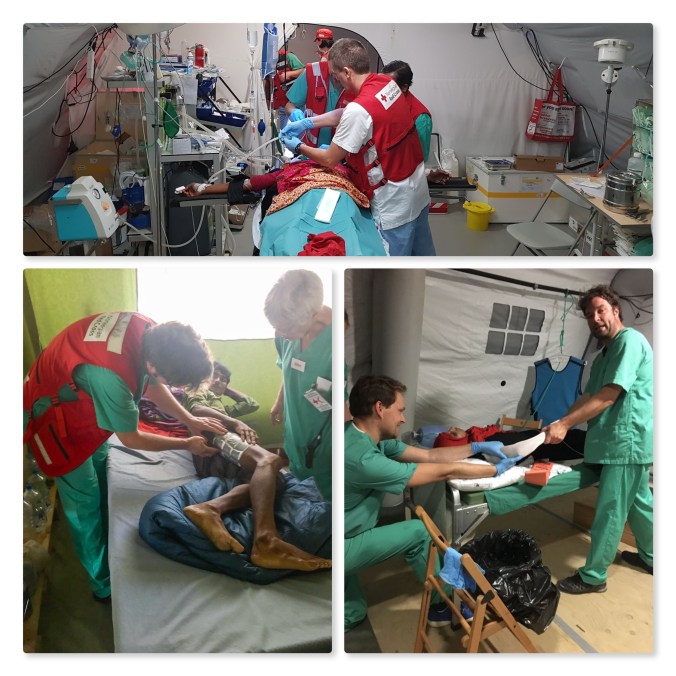
A normal day at work. A glimpse from the OT (top), ward rounds and dressing changes with duck tape (bottom left) and repositioning of fractures with Sigge, the Icelandic anesthesiologist and my brother in the OT (bottom right)
Surprisingly, there is hardly any violence in the refugee camps. In spite of the dire and desperate conditions the community seems to solve conflicts without resorting to violence. The village elders have maintained their considerable and calming influence, a remarkable feat considering that their people are uprooted and traumatized with virtually no prospect of improving their living conditions and a grim future ahead of them.
But there still is a lot of surgical trauma. This is largely due to traffic accidents because… well… people drive like maniacs. A very important public health initiative in Bangladesh with huge life-saving consequences? Answer: Driving lessons.
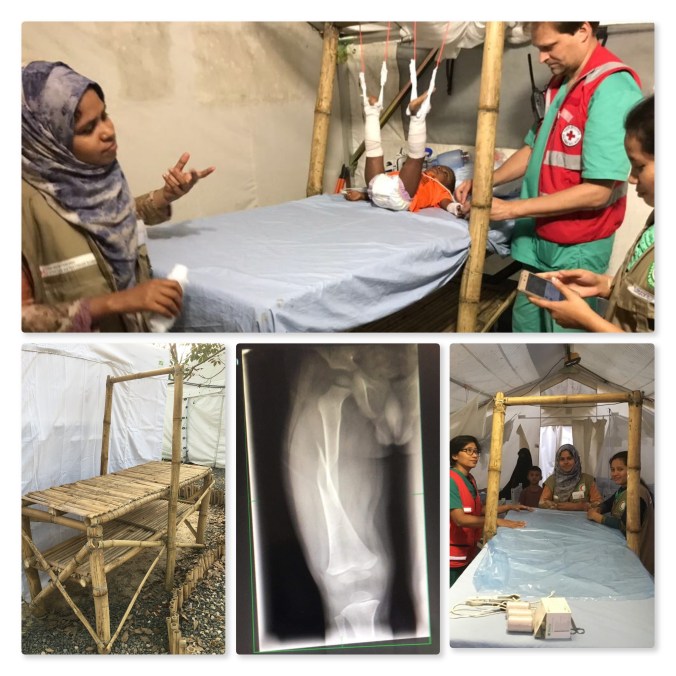
I asked the local technicians for a stretching gallow, in case we received any thigh fractures in children. They build me this whopper! An entire bed with a gallow and an extra shelf for tools! I never saw it in action, but the team after us put it to good use.
Base Camp
Danish Red Cross is in charge of our living quarters that consist of tents, field beds and mosquito domes. We have basic sanitary installations: Simple showers (cold), a sink and toilets (non-flushing). We have washing machines and a drier. Electricity is produced by diesel generators which struggle every now and again in the rain and humidity. Every team has a basic kitchen area with a refrigerator, a freezer and cooking plates. It is there we get to sit together in the evenings to chat and defuse.

Some photos of Base Camp. The formidable Brian Kit Wong from Hong Kong RC at the wash-your-troubles-away laundromat (Top), Pablo’s fitness and spa showers (bottom left), Viking village with the tents (bottom middle) and the sunrise at the kitchen area (bottom right)
There is also a canteen where everyone can buy warm food. I prefer the Norwegian dry food bags, but after 10 days we are out of those. Disease among the international delegates has been a hallmark of every rotation and safe food and water are essential for functioning. But the food in the canteen is decent and it hasn’t caused me any trouble on the diarrhea front!
For Xmas dinner the team leaders have organised a couple of goats and a butcher that comes along with them. I must admit that all I ever got out of these goats were bones and tendons, but everyone appreciated the effort. Xmas eve 2017 is certainly something I will remember for a long time. Every nation present (and there are quite a few!) has to perform a Xmas carol which is typical for their country. The Bangladeshis, probably due to a shortage of Xmas carols in this mainly Muslim country, top it all off with a couple of songs which, for the untrained ear, can sound a bit shrill and noisy but which would certainly win the day at any serious Asian Karaoke competition.

To preserve your sanity under difficult circumstances you need a sense of humour and some normalcy. Top right: Third sunday in Advent celebration, Bottom left: Xmas decoration, Bottom middle: Crazy Santas, Bottom right: Xmas dinner
The Team
We are surrounded by suffering, trauma, disease and despair. Including the local population there are approximately one million people who need – among many other things – medical care. You don’t need to be a statistician to realize that the resources we have at our disposal are not even close to covering the needs of the people around us, even if we worked twenty-four hours a day and seven days a week. Inevitably, ethical dilemmas, difficult decisions and tough calls have to be made on a daily basis. It is easy to get sucked into individual cases and use all your resources on them, particularly when the patient is a child. This is what we are trained for in Western medicine. It is not just in our blood. It is a bone marrow reflex, our second nature.
But following this reflex unquestioningly under these circumstances can get you into trouble. Because our mission doesn’t just last for a couple of days which would give us the opportunity to burn the candle in both ends and exhaust ourselves completely before heading home and sleeping it off for a couple of days. We are here for weeks and we will have to work long hours every day and this means that everyone will have to get some time off every day to relax and will have to get at least five hours of sleep every night. Why? Because you not only have to fight another day, but you will have to fight every day. You will have to make sure that you have enough energy to function every day, to cope with the challenges that will come your way every day and to make good and sound decisions every day. Otherwise, you may jeopardize not only your position, but the functioning of the entire team.
So how do you make this work in reality? How can you go to sleep when you know that there is a child in the ward that may not make it through the night? How can you get some time off in the evening when you have admitted a young woman during the day who has a serious condition that you cannot diagnose properly, who doesn’t respond to the treatment you give her and who may also die during the night?
I don’t know if there is a good answer to these questions. I only know what we did and it helped to ease the burden: We took it on as a team. I have always marvelled at the efforts Western corporations put into finding a motto for their company. They take the leaders on a weekend retreat, do lots of work-shops and they come back with catch phrases like Honesty, Reliability, Accountability, etc. which they then struggle to fill with life and proper meaning. I truly believe you only need one motto for a team that has to work under stress. It is borrowed from Liverpool FC: You never walk alone. I think we lived by this motto. We sat together in the evenings, discussed the difficult patients and made sure we had implemented everything we had to offer. We instructed the local doctors that were on call accordingly and then left it to them. It was a leap of trust, but it worked.

Impressions from the team on my rotation. Good people, local and expat, who I miss deeply. It has been an honour serving by their side.
We only spend a tiny fraction of a year together before we go back to our normal lives. We have often never met before and we may not ever meet again. This is part of being on a mission. But it is an intense time and the challenges that we have to face together and the problems that we solve every day quickly turn strangers into family. I for my part feel privileged and proud to be part of this family.
Afterthought
It has been a tough and demanding mission. When I walked through the camps I couldn’t quite shake the feeling that I can probably return in fifteen or twenty years and meet exactly the same conditions. There are few signs that Hope may one day return to these shelter-dotted hillsides.
The field hospital is going to continue its work for at least the rest of 2018 and it will need funding. Please remember that this crisis is not going to go away although it will most likely not get much media attention! Donating money WILL make a difference on the ground. This is the link to Norwegian Red Cross homepage where you can make your contribution. Other national Red Cross societies have similar links for donations. It is greatly appreciated and needed!
Read also my blogs on previous missions:
.……and my attempt at giving a fair and balanced picture on prostate cancer:
Excellent article written by my brother in law! I am so proud that you are part of my family! Yours sincerly Guri
Such an I ncredibly moving account Sven it’s so easy to forget the 24/7 need for compassion, expertise and money to keep this amazing work going.
Everyone involved out there (& in other parts of the world in similar situations) is awe inspiring. Massive respect. Jo x
Kudos, Sven,
Thank you!
Pingback: Prostate Cancer for Dummies- Part 1: Basics | Journeys in Medicine
Pingback: Prostate Cancer for Dummies-Part 2: the PSA | Journeys in Medicine
Pingback: The Earthquake in Nepal. Looking back | Journeys in Medicine
Pingback: THE PHILIPPINES AFTER YOLANDA- PART 1 | Journeys in Medicine